Restrictive diets are often evaluated by what they remove. Calories are reduced, food groups are eliminated, and eating windows are narrowed. Success is typically measured by weight change, blood markers, or adherence. What is less frequently examined is how restriction alters the body’s internal balance of minerals that regulate hydration, nerve signaling, muscle contraction, and energy use.
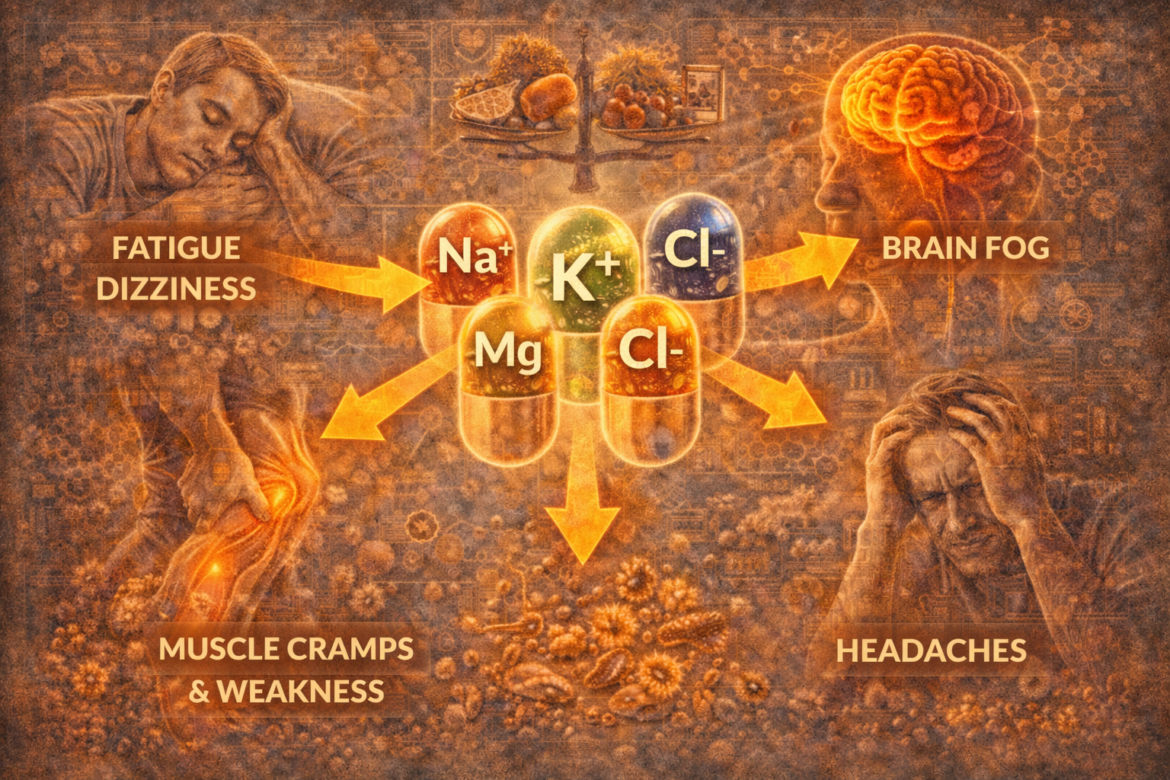
Electrolytes, including sodium, potassium, magnesium, and chloride, play a foundational role in physiological stability. When intake patterns shift abruptly or remain constrained over time, electrolyte balance can deteriorate even in the absence of obvious malnutrition. Increasingly, clinicians and researchers are recognizing electrolyte depletion as an early and underappreciated consequence of restrictive dietary patterns.
Understanding how electrolyte depletion develops and how it presents before severe deficiency occurs helps explain why some individuals experience fatigue, dizziness, or weakness despite meeting calorie or protein targets.
What Electrolytes Do in the Body
Electrolytes are minerals that carry an electrical charge when dissolved in bodily fluids. This charge allows them to regulate nerve impulses, muscle contractions, fluid distribution, and acid-base balance.
Sodium and potassium maintain electrical gradients across cell membranes. Magnesium stabilizes ATP, the molecule that fuels cellular work, and regulates hundreds of enzymatic reactions. Chloride contributes to fluid balance and digestive function.
These minerals are not optional or interchangeable. They operate as a coordinated system, and an imbalance in one often disrupts the others. Because electrolytes are continuously lost through urine, sweat, and respiration, regular replenishment is essential.
Why Restrictive Diets Increase Risk
Restrictive diets alter electrolyte balance through multiple mechanisms. Reduced food volume lowers total mineral intake. Elimination of entire food groups may remove primary sources of specific electrolytes. Changes in insulin signaling and hydration further accelerate losses.
Low-carbohydrate and very-low-calorie diets reduce insulin levels, which increases sodium and water excretion by the kidneys. As sodium is lost, potassium and magnesium often follow. Fasting protocols amplify this effect by extending periods without intake.
Importantly, these changes can occur even when a diet is nutritionally intentional. Electrolyte depletion is not limited to extreme or disordered eating. It can develop gradually in structured dietary plans that emphasize restriction without adequate mineral replacement.
Early Signs Often Appear Subtle
The early signs of electrolyte depletion are frequently nonspecific. Fatigue, lightheadedness, headaches, muscle tightness, or reduced exercise tolerance may emerge without clear cause.
Because these symptoms overlap with common adjustment effects during dietary change, they are often dismissed as temporary or psychological. However, they reflect measurable physiological changes.
Research summarized by the National Institutes of Health notes that mild electrolyte imbalances can impair neuromuscular function and cardiovascular regulation long before laboratory values fall outside reference ranges.
This explains why individuals may feel unwell despite “normal” test results.
Sodium Loss and Circulatory Symptoms
Sodium plays a central role in maintaining blood volume and pressure. Early sodium depletion reduces plasma volume, leading to dizziness upon standing, weakness, or a sense of low energy.
In restrictive diets, sodium loss often accelerates due to increased urinary excretion. This is especially common when carbohydrate intake drops or fasting periods lengthen.
Reduced blood volume also affects nutrient delivery and thermoregulation, contributing to cold sensitivity and fatigue. These symptoms are often mistaken for calorie deficiency rather than electrolyte imbalance.
Potassium and Muscle Function
Potassium regulates muscle contraction and nerve signaling. Even modest reductions can impair muscle performance, leading to cramping, twitching, or early fatigue.
Restrictive diets may reduce potassium intake by limiting fruits, vegetables, or legumes, common dietary sources. At the same time, increased sodium loss promotes potassium excretion.
Early potassium depletion may not produce dramatic symptoms, but it reduces exercise capacity and prolongs recovery, particularly during physical activity or heat exposure.
Magnesium and Energy Stability
Magnesium is involved in energy production, nerve conduction, and muscle relaxation. It stabilizes ATP and supports enzymatic reactions required for metabolic efficiency.
Low magnesium availability often presents as muscle tightness, poor sleep quality, irritability, or persistent fatigue. These symptoms are frequently attributed to stress or adaptation to diet rather than mineral depletion.
Harvard Health Publishing has noted that marginal magnesium intake is common and that symptoms often appear before deficiency is clinically diagnosed, particularly during dietary restriction.

Hydration Without Electrolytes
One of the most common contributors to electrolyte depletion is increased fluid intake without corresponding mineral replacement. Individuals following restrictive diets often increase water consumption to manage hunger or support fasting.
While hydration is essential, excess water dilutes circulating electrolytes when intake is not balanced. This dilution exacerbates sodium and potassium loss, worsening symptoms.
This dynamic helps explain why some individuals feel worse when they “drink more water” during restrictive eating phases.
Nerve Signaling and Cognitive Effects
Electrolytes are essential for neural communication. Early depletion can impair signal transmission, leading to brain fog, reduced concentration, and slowed reaction time.
These cognitive effects are often subtle but impactful. They may appear as reduced motivation, difficulty focusing, or mental fatigue, particularly during prolonged restriction.
Because these symptoms are not dramatic, they are rarely linked to electrolyte status unless a more severe imbalance develops.
Restriction, Stress Hormones, and Electrolyte Loss
Restrictive diets increase physiological stress, even when intentional. Stress hormones influence kidney function and fluid regulation, promoting electrolyte excretion.
Elevated cortisol increases sodium loss and alters potassium handling. Combined with dietary restriction, this hormonal environment accelerates depletion.
This interaction explains why electrolyte symptoms often intensify during periods of psychological stress or increased physical demand.
Why Deficiency Often Goes Unrecognized
Electrolyte depletion is difficult to detect early because blood levels are tightly regulated. The body prioritizes maintaining serum concentrations, even at the expense of intracellular stores.
As a result, laboratory tests may appear normal while tissues experience a functional shortage. Symptoms emerge from cellular imbalance rather than overt deficiency.
This gap between laboratory assessment and lived experience contributes to underrecognition of electrolyte depletion in restrictive diets.
Restrictive Diets and Cumulative Loss
Electrolyte depletion is rarely caused by a single meal or short-term fast. It develops cumulatively as intake remains insufficient and losses persist.
Over time, small imbalances compound. Recovery becomes slower. Physical resilience declines. The body operates closer to its regulatory limits.
From a nutritional deficiency perspective, this cumulative effect is more relevant than acute deficiency events.
A Preventive Perspective on Electrolytes
Modern nutrition research increasingly emphasizes prevention rather than correction. Addressing electrolyte balance early prevents downstream consequences such as cardiovascular strain, neuromuscular dysfunction, and reduced metabolic efficiency.
Resources focused on metabolic and nutritional health, including those offered by Dr. Berg, frequently stress the significance of being aware of electrolytes during dietary restrictions, treating them as a crucial factor rather than a secondary concern.
Rethinking Restriction and Nutrient Sufficiency
Restrictive diets are often evaluated solely on macronutrient composition. Electrolyte depletion highlights the limitation of this approach.
Adequate calories and protein do not guarantee mineral sufficiency. Diets that reduce food diversity or volume must account for micronutrient and electrolyte needs explicitly.
This reframing shifts dietary evaluation from what is removed to what must be maintained.
Implications for Nutritional Guidance
Recognizing early electrolyte depletion has implications for dietary guidance, especially in weight loss, fasting, and elimination-based approaches.
Rather than reacting to severe symptoms, monitoring early signs allows for proactive adjustment. This aligns with a broader trend in nutrition science toward functional markers rather than crisis management.
Electrolyte balance supports performance, cognition, and metabolic stability, making it a foundational aspect of nutritional adequacy.
Electrolyte depletion is an early and often overlooked consequence of restrictive diets. Its symptoms are subtle, cumulative, and frequently misattributed to adaptation or discipline.
Understanding electrolyte depletion as a physiological response to altered intake and hormonal signaling clarifies why fatigue, dizziness, and weakness can emerge even in carefully planned diets.
As dietary patterns continue to evolve toward restriction and optimization, maintaining electrolyte balance will remain essential for preserving function, resilience, and long-term health.